The case
A 15 year old skateboarder totally screws up a rail grind. After posting his wipeout to YouTube his friends call his mom, who notices that he has been unable to walk on his ankle – probably because of how ridiculously swollen it is.

A gnarly swollen ankle
You get an XRay, because that’s what you do…

The ankle X-Ray you just got
The Diagnosis
Hmm, doesn’t look that bad right? Right? OK, this is an educational blog, so yes, it is bad. This is a big deal fracture. In fact it is a Salter-Harris IV fracture of the distal tibia. AKA the dreaded Triplane Fracture.

The fracture plane of this triplane fracture
Why is it so bad? Well, aside from being accountable for 10% of the intra-articular ankle fractures in patients with open physes. Boys predominate, probably because they like to do things like rail grind on their skateboards. The peak age is 12-15 years. The fracture itself involves three planes:
- Transverse through the physis
- Sagittal through the epiphysis
- Coronal through the distal tibial metaphysis
This diagram may help.

3D representation of the planes of the triplane fracture
The main concern is not growth arrest, but rather the stability of the articular surface itself. That should lead you to assume (correctly) that these fractures generally need to be stabilized in the OR. More on that in a minute (of your reading time).
Management
As you can see from the initial X-Ray the initial findings are not 100% obvious in many cases. However it is still important to get them first (after applying the Ottawa ankle rules of course) as is a high level of association with concomitant fibula fractures. Normal ankle X-Rays show the ‘telephone’ sign, where the tibia and fibula (the handset) sit above the talus (the telephone base).
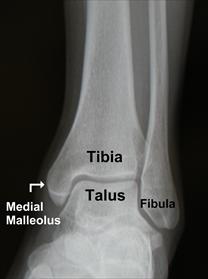
A normal looking ankle X-Ray
Asymmetry, and disruption to this normal orientation suggests a fracture. This is one fracture where a CT scan can be helpful, especially with the new 3D reconstruction modalities. Establishing the plane of disruption can be very helpful for your orthopedic colleagues.

Standard CT views in a triplane fracture

A really cool 3D reconstruction of a triplane fracture
In general orthopedists will first pursue closed reduction. Then, if a residual fracture gap of >2 mm exists surgical fixation is generally necessary. The likelihood of successful closed reduction (without need for surgery) is actually more likely if there is >3 mm of displacement initially. That doesn’t mean that you don’t have a role in the ED. Ater a careful neurovascular assessment you can provide pain medicines (these hurt quite a bit) and if transfer to another facility is warranted, place a posterior splint. These fractures should be seen urgently (within 24 hours) by an orthopedist.
For more information check out:
Ortho Bullets – Triplane Fractures







